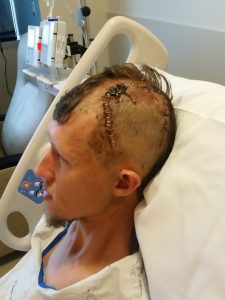
 After Kraston was newly diagnosed, I spent the following 3 days (while he was still in the hospital recovering from his brain surgery) researching glioblastoma treatment options.
After Kraston was newly diagnosed, I spent the following 3 days (while he was still in the hospital recovering from his brain surgery) researching glioblastoma treatment options.
Clinical Trials
The very Sunday before his diagnosis, 60 Minutes aired a story about a promising glioblastoma treatment from Duke University involving the polio vaccine. Many people shared this information while we were in the hospital.
I discovered that this treatment was a phase 1 trial for recurrent glioblastoma. Phase 1 means the trial is new and experimental, testing for the optimal dose. Recurrent means the tumor has to have started growing again after treatment for a newly diagnosed tumor, meaning he did not (yet) qualify.
I did a little bit more research and compiled the following considerations:
- There are many more clinical trials for recurrent glioblastoma than for newly diagnosed glioblastoma.
- Most recurrent glioblastoma trials have the standard treatment as a prerequisite.
- Some newly diagnosed trials included treatment that could exclude you from the more promising recurrent trials.
- Most newly diagnosed trials included the standard treatment with simply an additional experimental drug added. Nothing overly groundbreaking jumped out during my research.
- No trials were recruiting in Tulsa, meaning we would have to travel or live away from home for treatment.
- Our 4th child was expected before he would finish radiation.
Taking these factors into account, we determined that we would complete the standard treatment with home town oncologists. If he had a recurrence, we could consider a recurrent clinical trial like the Duke polio vaccine trial at that time.
Standard Treatment
A radiation oncologist and a medical oncologist each visited us describing the current ‘gold standard’ glioblastoma treatment options. We did meet with another radiation oncologist for a second opinion, who basically proposed the same radiation treatment. So at that time, there were three components to this standard treatment:
- Standard brain radiation therapy
- Concurrent temozolomide
- Adjuvant temozolomide
Brain radiation therapy
 Radiation is measured in either a unit called a gray (Gy) or a unit called a millisievert (mSv). 1 gray (Gy) = 1000 millisievert (mSv). For reference, a chest X-ray is approximately 0.1 mSv.
Radiation is measured in either a unit called a gray (Gy) or a unit called a millisievert (mSv). 1 gray (Gy) = 1000 millisievert (mSv). For reference, a chest X-ray is approximately 0.1 mSv.
Based on the size of his tumor, the standard is (33) treatments of 1.8 Gy fractions, for a total exposure of 59.4 Gy. So his radiation exposure would be approximately equivalent to 594,000 chest X-rays.
He would receive one treatment per weekday, so the 33 treatments would take him just shy of 7 calendar weeks to complete. The type of procedure was called intensity modulated radiation therapy (IMRT) and only took 10-15 per day.
The main side effect of the radiation was hair loss. His radiation oncologist recommended putting an ice pack on his head before and after the radiation in order to prevent permanent hair loss.
Concurrent Temozolomide
Starting the same day as the radiation, he would start taking an oral chemotherapy called temozolomide (TMZ) every single day until he stopped radiation. Since TMZ is a pill, he would get a prescription filled at a pharmacy and take the pill each night at home. He did not have to go anywhere for an infusion like most other chemotherapy.
The main side effect of TMZ is nausea. Kraston’s regimen to mitigate the nausea was the following:
- One hour before bed, take 8mg of ondansetron (generic of Zofran, expensive anti-nausea drug developed primarily for chemo patients)
- At bedtime, take his TMZ dose.
- The next morning, take 10mg prochlorperazine (generic of Compazine, cheap older anti-nausea drug).
Adjuvant Temozolomide
One month after radiation ended, he would start adjuvant temozolomide. He got a new prescription for twice the original strength of the chemo pills. For 5 straight days each month, he would take this new dosage. He would do this for 6 months. The same regimen of anti-nausea medicines have worked for the increased dosage.
Novocure Optune
 When Kraston was first diagnosed, the Novocure Optune had only recently received FDA approval for use by newly diagnosed glioblastoma patients. It was not until after he completed his radiation that the National Comprehensive Cancer Network (NCCN) announced their recommendation that the Novocure Optune device be added to the standard glioblastoma treatment options.
When Kraston was first diagnosed, the Novocure Optune had only recently received FDA approval for use by newly diagnosed glioblastoma patients. It was not until after he completed his radiation that the National Comprehensive Cancer Network (NCCN) announced their recommendation that the Novocure Optune device be added to the standard glioblastoma treatment options.
The optune device consists of 4 arrays hydrogelled to his head, with cords connecting to the device in his backpack. The device creates tumor treating electrical fields which confuse the cancer cells. They get so confused that they forget to reproduce and die off, reducing the total number of cancer cells.
There are only a few radiation oncologists who have trained with Novocure and are permitted to prescribe the Optune. Part of the reason we choose the radiation oncologist that we did was because he had this option available for Kraston.
The main side effect of this treatment is skin irritation. Kraston’s hasn’t been too bad.He has been able to maintain wearing the arrays approximatelt 90% of the time.
Newly Diagnosed Glioblastoma Treatment Options
So there you have the glioblastoma treatment options for a newly diagnosed patient. At the time of publication of this post, Kraston has completed radiation and concurrent TMZ, 5 of the 6 cycles of adjuvant TMZ and 3+ months of Optune treatment.
Since his is coming up on 6 months progression free survival after completion of radiation, he has responded well so far to the standard treatment.
Amanda this is awesome & I’m so happy you have created this blog. We love you all & continue to pray for Kraston & all of you.
Thanks, Susie. I am finding it really cathartic to write some of this out. Thank you for the prayers and love you too.
How it goes so far ?
Thanks for this info btw
Aziz,
Thank you for your post. Unfortunately my husband passes away in April from complications after his second surgery. You can read my mini-update here.
Amanda